Discover what pediatric dermatology is and how specialized care can effectively address your child's unique skin issues for better outcomes.
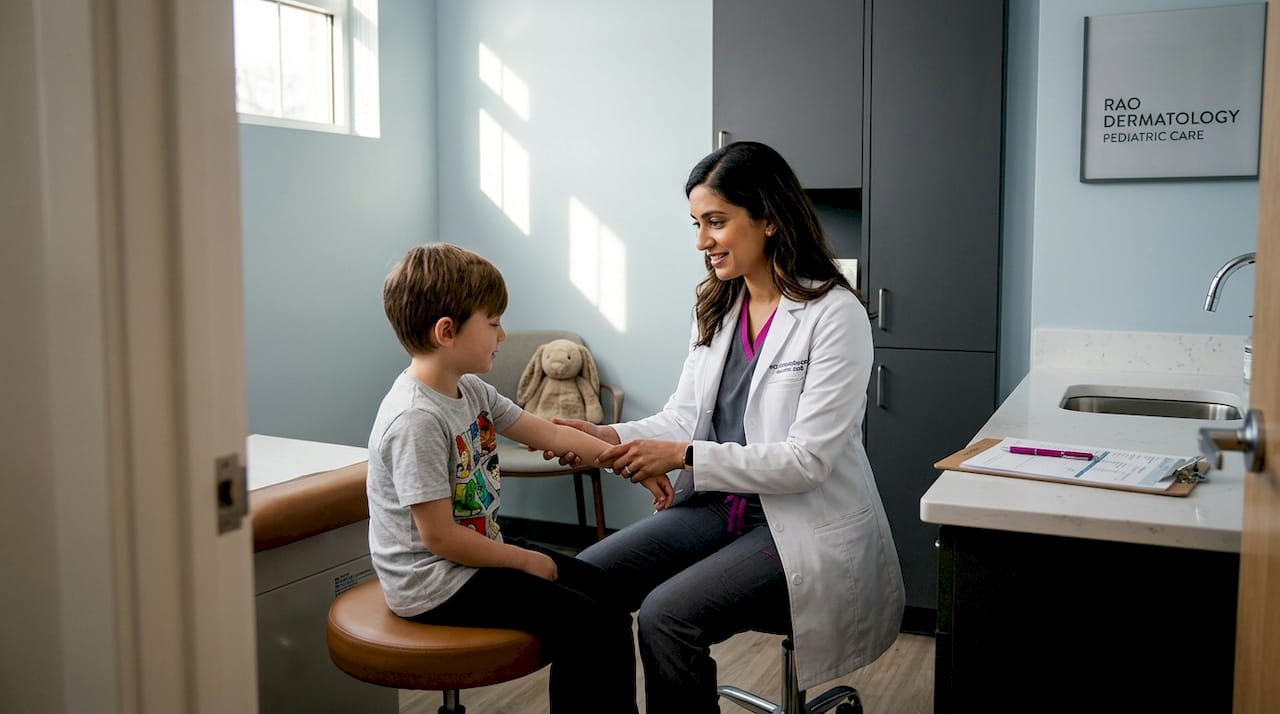
Most parents assume any dermatologist can handle their child’s skin problems. It seems logical enough. But children’s skin is not simply a smaller version of adult skin. It behaves differently, responds differently to treatment, and develops conditions that require a completely different kind of expertise. Pediatric dermatology is the subspecialty dedicated entirely to diagnosing and managing skin conditions from birth through adolescence, and choosing this level of care for your child can make a meaningful difference in outcomes.
Table of Contents
- The role of a pediatric dermatologist
- How pediatric dermatology differs from general dermatology
- Common childhood skin conditions treated
- When to see a pediatric dermatologist
- Why specialized pediatric skin care matters more than you think
- Find advanced pediatric skin care you can trust
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Specialized pediatric care matters | Children’s skin needs expert attention different from adult dermatology. |
| Additional training is essential | Pediatric dermatologists complete special training and board certification. |
| Range of childhood skin conditions | Common issues treated include eczema, birthmarks, warts, and psoriasis. |
| Knowing when to seek help | Chronic or unusual skin changes in children often require a pediatric dermatologist’s expertise. |
The role of a pediatric dermatologist
Pediatric dermatology is not just general dermatology applied to younger patients. It is a recognized medical subspecialty with its own body of knowledge, its own training pathways, and its own approach to patient care. The entire focus is on understanding how skin develops, changes, and responds during childhood and adolescence.
As HealthyChildren.org notes, pediatric dermatology covers patients from the newborn stage through the teenage years. That is a wide range, and the skin conditions seen in a three-month-old are radically different from those seen in a 16-year-old. A practitioner who specializes in this age range understands those distinctions in a way a general dermatologist simply may not.
The conditions pediatric dermatologists manage every day include:
- Atopic dermatitis (eczema): One of the most common childhood skin conditions, characterized by itchy, inflamed patches
- Birthmarks: Including port-wine stains, hemangiomas, and congenital nevi, some of which require early intervention
- Warts: Caused by the human papillomavirus, often spreading quickly in school-age children
- Psoriasis: Presents differently in children than in adults, often appearing on the scalp, face, and skin folds
- Seborrheic dermatitis: Commonly called “cradle cap” in infants
- Tinea (ringworm): A fungal infection that spreads easily among children in group settings
- Molluscum contagiosum: A viral skin infection particularly common in young children
“Pediatric dermatology is the subspecialty focused on diagnosing and managing children’s skin conditions, from birth through adolescence.” — HealthyChildren.org
Exploring pediatric dermatology care gives you a clearer picture of how this specialized approach translates into better, safer treatment for your child.
Beyond treating skin disease, pediatric dermatologists also play an important role in early detection. Certain birthmarks or pigmented lesions that appear benign at first glance can carry risk. A specialist trained to evaluate these presentations has the clinical background to know when to watch, when to biopsy, and when to intervene.
How pediatric dermatology differs from general dermatology
Understanding what sets pediatric dermatologists apart goes beyond a simple comparison of credentials. It involves understanding how training shapes clinical thinking and how a child-centered approach changes the entire experience of care.

Training and certification
General dermatologists complete medical school followed by a residency in dermatology, typically three years. That training is thorough and covers a wide spectrum of conditions. But pediatric dermatologists go further. They complete an additional fellowship in pediatric dermatology after their residency, then earn subspecialty board certification through the American Board of Dermatology. That additional layer of training is focused entirely on children’s skin.

Here is a direct comparison:
| Feature | General dermatologist | Pediatric dermatologist |
|---|---|---|
| Residency training | 3 years | 3 years |
| Fellowship | Optional or different focus | Required: pediatric dermatology |
| Board certification | American Board of Dermatology | Plus subspecialty pediatric board cert |
| Primary patient focus | Adults and some children | Newborns through adolescents |
| Familiarity with pediatric conditions | Variable | Extensive and specialized |
| Communication approach | Standard clinical | Child-adapted, family-centered |
| Procedural tools/dosing | Adult-calibrated | Adjusted for size and age |
Knowing the difference between medical vs cosmetic dermatology can also help parents understand which type of specialist and which type of visit their child actually needs.
Approach to child patients
It is not only about knowledge. A pediatric dermatologist’s office looks and feels different. Procedures are designed with a child’s comfort in mind. Topical anesthetics are used more consistently. Explanations are given to both the parent and the child at an appropriate level. Waiting rooms, exam tables, and even the tone of conversation are calibrated to reduce fear and build trust.
Children do not always communicate pain or discomfort the way adults do. A specialist trained to work with this population reads behavioral cues, understands developmental stages, and knows how to work quickly and efficiently to minimize distress. That matters enormously when you have a frightened six-year-old who needs a skin procedure.
Pro Tip: When scheduling your child’s first visit with any dermatologist, ask directly whether they have completed a pediatric dermatology fellowship. Board certification in the subspecialty is your clearest signal that the provider has the specialized training your child deserves.
Common childhood skin conditions treated
Now that you understand the specialist’s training and approach, it helps to see exactly which conditions bring children to a pediatric dermatologist most often, and why specialized expertise actually changes outcomes.
The most common pediatric conditions treated include eczema, psoriasis, warts, and birthmarks. Each of these requires a level of clinical nuance that goes well beyond what most parents expect.
| Condition | Common symptoms | Specialized treatment approach |
|---|---|---|
| Atopic dermatitis (eczema) | Itchy, red, dry, or weeping patches | Age-appropriate topical agents, wet wrap therapy, allergen identification |
| Psoriasis | Thick, scaly plaques, often on scalp/face | Child-adjusted dosing of biologics or topicals |
| Warts | Rough, raised bumps on hands or feet | Cryotherapy calibrated for sensitive skin |
| Hemangiomas (birthmarks) | Red or purple raised marks, often growing in infancy | Propranolol therapy, laser treatment, watchful waiting |
| Molluscum contagiosum | Small, dome-shaped bumps | Topical immunotherapy or physical removal |
| Seborrheic dermatitis | Scaling on scalp or face | Gentle antifungal shampoos or mild topical steroids |
Understanding the differences between psoriasis and eczema is particularly useful for parents because these two conditions are frequently confused. Both involve red, inflamed skin, but they differ in cause, location, texture, and treatment. A misdiagnosis between the two leads to ineffective treatment and unnecessary suffering for your child.
It is also worth noting the connection between diet, allergies, and skin symptoms. Research shows that certain foods can trigger or worsen conditions like eczema in sensitive children. Food intolerance and skin issues are closely linked, and a pediatric dermatologist often works collaboratively with allergists or pediatric gastroenterologists to identify and address those triggers. This integrated approach simply does not happen as consistently in a general dermatology setting.
Additional conditions managed under medical dermatology services include contact dermatitis, vitiligo, and even early skin cancer detection in adolescents. These are not rare edge cases. They are real concerns that require real expertise.
Some conditions children face include:
- Vitiligo: Loss of skin pigmentation that can have significant psychological impact on older children and teens
- Alopecia areata: Patchy hair loss with immune-mediated causes that can be distressing for school-age children
- Acne: Particularly in preteens and teens, where early treatment prevents scarring
- Contact dermatitis: Often triggered by diapers, soaps, or metals like nickel
When to see a pediatric dermatologist
Pediatric dermatologists treat children from birth through adolescence, and there is no minimum age to seek evaluation. Parents often wait too long, assuming a skin issue will resolve on its own or that a pediatrician’s assessment is sufficient. Sometimes that is true. But several clear signs indicate your child needs a specialist.
- A rash or skin condition that has persisted for more than two to three weeks without improvement despite over-the-counter treatment
- A birthmark that changes in size, color, or texture over time, or one that bleeds without injury
- Recurring skin infections in the same area or spreading to multiple areas
- Eczema or rashes that interfere with sleep, school, or daily activities because of itching or discomfort
- Skin symptoms paired with other health changes such as joint pain, fever, or fatigue, which may signal a systemic condition
- A diagnosis of psoriasis or eczema from a general practitioner that is not responding to treatment
- Any suspicious lesion or pigmented spot in an adolescent who has had significant sun exposure or a family history of melanoma
When you are ready to book a visit, ask the practice a few key questions. Confirm the provider has completed fellowship training in pediatric dermatology. Ask about their experience with your child’s specific condition. Inquire whether they use pediatric-appropriate dosing and equipment for any procedures. These questions are not excessive. They are exactly what a good specialist expects from an engaged parent.
Pro Tip: If your child’s general practitioner has already tried two or more treatments without success, do not wait for a third round. That pattern is a clear signal that specialized evaluation will save time, money, and your child’s comfort.
Learning more about how to find a pediatric dermatologist with the right credentials and experience is a practical first step before you make an appointment.
Why specialized pediatric skin care matters more than you think
Here is the honest truth most articles on this topic avoid. Parents are often told that any board-certified dermatologist can handle their child’s skin. And technically, many can manage straightforward cases. But the gap between “technically capable” and “optimally trained” can be significant, and children pay the price for that gap.
We see this pattern regularly. A child with moderate to severe eczema is prescribed adult-strength topical steroids at too high a concentration for too long, leading to skin thinning (atrophy) in a child whose skin is far more permeable than an adult’s. A birthmark is dismissed as cosmetically benign when clinical monitoring over time would have revealed growth patterns worth investigating. Psoriasis in a child is treated with the same regimens used for adults, without accounting for the weight-based dosing adjustments that prevent systemic side effects.
These are not hypothetical. They are consequences of applying adult dermatology protocols to pediatric patients without the additional training to know when those protocols need modification.
The treatments for psoriasis and eczema in children involve considerations that simply do not exist in adult care. The surface-area-to-body-weight ratio is higher in young children, meaning topical medications are absorbed more readily. That changes the safety calculus entirely.
There is also a psychological dimension that specialized providers understand better. Chronic skin conditions during childhood affect self-esteem, social development, and academic performance. A pediatric dermatologist is trained to consider the whole child, not just the skin finding. They communicate with schools, coordinate with mental health professionals, and counsel families on how to help children cope with visible conditions in a way that supports long-term wellbeing.
Relying on self-treatment or delaying specialist referral is one of the most common patterns we see, and it almost always extends suffering unnecessarily. Early, expert intervention produces better outcomes for chronic conditions like eczema and psoriasis. It leads to fewer flares, less reliance on high-potency medications, and a better quality of life for both the child and the entire family.
Find advanced pediatric skin care you can trust
Your child’s skin is not just a cosmetic concern. It is a critical organ, and its health affects how your child feels, sleeps, socializes, and grows. When a skin condition is chronic, recurring, or simply not responding to standard treatment, the right next step is a specialist who has dedicated their career to children’s dermatology needs.
At Rao Dermatology, our board-certified team brings over 25 years of dermatological expertise across our New Jersey, New York, and California locations. We offer Pediatric Dermatology services designed specifically for young patients, with a child-centered approach that makes evaluation and treatment as comfortable as possible. From eczema and psoriasis to birthmarks and warts, our providers have the specialized training your child deserves. Explore our full range of all dermatology services to learn more about what we offer and find the location nearest to you.
Frequently asked questions
What ages do pediatric dermatologists treat?
Pediatric dermatologists treat children from birth through adolescence, covering every developmental stage from newborn to teenager.
Does my child need a referral to see a pediatric dermatologist?
Referral requirements depend on your specific insurance plan and primary care provider, but many pediatric dermatology practices accept direct appointments without a referral.
Are pediatric skin conditions different from adult ones?
Yes. Children’s skin conditions differ from adult presentations in cause, location, appearance, and treatment response, making specialized training essential for accurate diagnosis and effective care.
How are pediatric dermatologists certified?
They complete a pediatric dermatology fellowship after their residency and then earn subspecialty board certification through the American Board of Dermatology, beyond the standard dermatology board certification.
What are the most common skin conditions treated by pediatric dermatologists?
Eczema, psoriasis, warts, and birthmarks are among the most frequently treated conditions, along with molluscum contagiosum, seborrheic dermatitis, and tinea infections.
